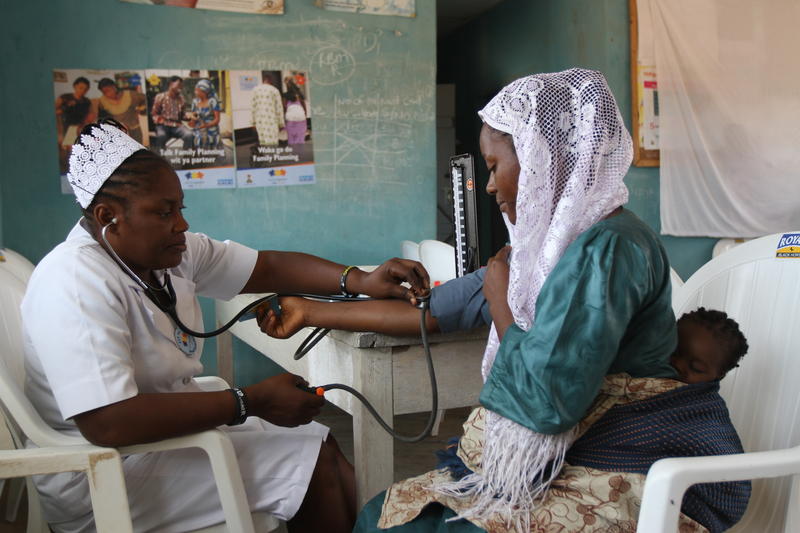
Asking a woman about her contraceptive preferences, providing information on all options and putting in place follow-up plan may significantly improve the chances that she will adopt a long-acting family planning method, new Johns Hopkins Center for Communication Programs research suggests.
Published recently in the International Journal of Gynecology and Obstetrics, the findings from Nigeria show that improved patient-provider communication can increase the chances that a woman will adopt a long-acting contraceptive method by 16 percent.
“Counseling is key,” says Stella Babalola, PhD, the study’s principal investigator and acting director of research and evaluation at CCP. “When providers counsel women in a deliberately client-centered way, when they clearly explain options and answer questions, women are significantly more likely to choose a method that is best for them, which is often a long-acting one.”
Long-acting reversible contraception, known as LARCS, include intrauterine devices (IUDs) and hormonal implants. LARCs are the most effective methods available to women, as they don’t depend on user adherence and have a reduced risk of failure as compared to short-term or traditional methods.
Nigeria is one of the most populous countries in the world and the fertility rate remains high at 5.5 deliveries per woman. In 2013, 15 percent of women there reported having unwanted pregnancies. Currently, the adoption of contraceptive methods remains low, with only 10 percent of married women of reproductive age using any contraceptive method and less than 2 percent using LARCs. Discontinuation of short-term methods such as oral or injectable contraceptives is high.
For this facility-based research, investigators interviewed 597 women between the ages of 18 and 49 at family planning sites in Kaduna and Ibadan, Nigeria, between June 1 and July 31, 2014. These women came seeking contraception.
Researchers asked questions to assess patient-provider communication by using what is known as the GATHER index, an assessment of the quality of family planning counseling that stands for Greet, Ask, Tell, Help, Explain and Return. The provider should greet the client warmly, ask questions about her desires for family planning, tell the client her options and provide information, help her select the best method, explain the method chosen including any potential side effects and make plans for the client to return to the clinic for follow up.
Those women whose counselors scored higher on the GATHER index were more likely to have adopted a LARC. The elements of Ask, Tell and Return were particularly important in determining whether a woman chose a LARC.
Other predictors of a woman’s adoption of a LARC include joint decision-making with her husband and a strong desire to avoid a pregnancy, but the importance of counseling on the decision was still evident even after controlling for those factors.
“We absolutely must increase the uptake of LARCs and this research shows that high-quality counseling can make a difference,” Babalola says. “Programs must strengthen the counseling skills of providers in order to see more women using the most appropriate contraceptive methods.”
“Healthcare provider interaction and other predictors of long-acting reversible contraception adoption among women in Nigeria” was written by Naira Kaira, John Ayankola and Stella Babalola. The research was funded by the Bill & Melinda Gates Foundation.