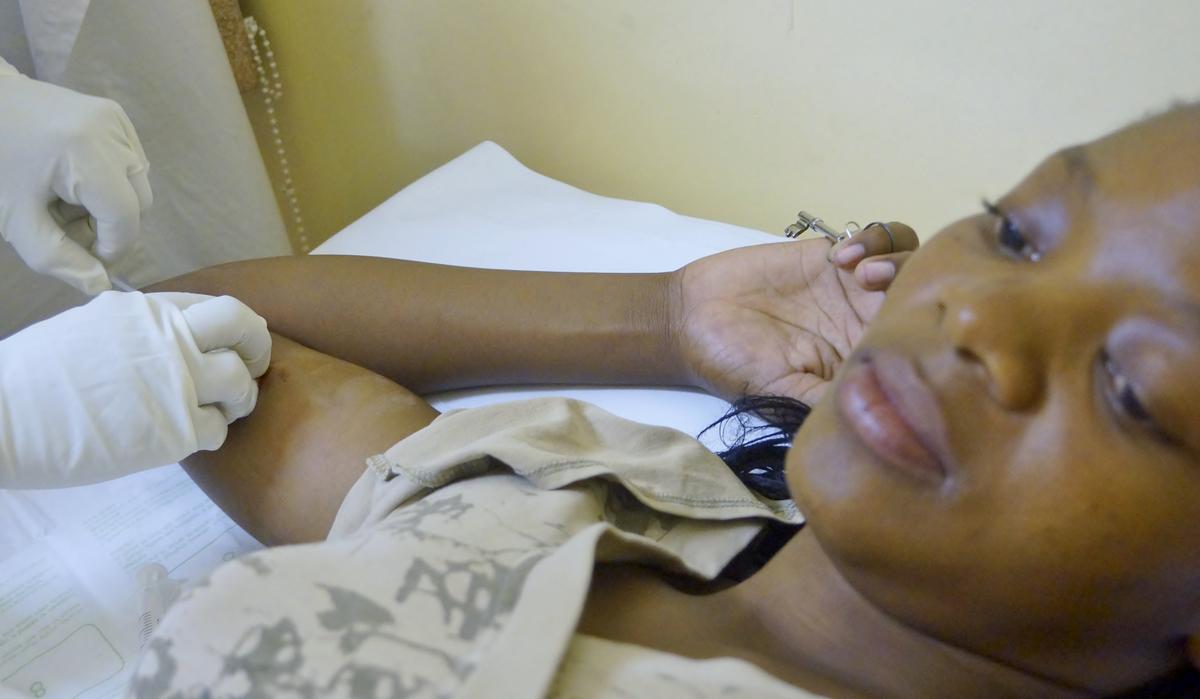
Results from a large clinical trial conducted in parts of Africa where HIV is highly prevalent and published today in the Lancet show that none of three long-acting and effective forms of contraception studied increased the risk that a woman using it would become infected with the virus.
But the study also raises concerns, finding that despite the high-quality HIV-prevention counseling that every woman in the trial received, the rate of new HIV infections remained alarmingly high.
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) trial was designed to determine whether there is a link between use of specific contraceptives and HIV acquisition. Beginning in 2015, more than 7,800 sexually active HIV-negative women in four countries – Eswatini, Kenya, South Africa and Zambia – were randomized by computer to receive one of three modern contraception methods: A progestogen-only injectable (Depo-Medroxyprogesterone Acetate intramuscular (DMPA-IM), a levonorgestrel implant (Jadelle) or a copper IUD. The women, whose average age was 23, were then followed by researchers for up to 18 months.
“An important message here is that in-service counseling alone – even high-quality counseling – is not enough,” says Susan Krenn, executive director of the Johns Hopkins Center for Communication programs.
The results make clear, Krenn says, that effective HIV prevention efforts require attention to entrenched social and structural issues that make it so difficult for women to follow through on.
“Gender and other social norms, systemic inequalities, power hierarchies, women’s agency to use condoms or access PrEP [pre-exposure prophylaxis medication] – all of these need to be addressed alongside high-quality counseling for family planning and HIV risk reduction,” she says.
The trial took place in areas where HIV infections are highly prevalent and found high rates of new infections among the women who participated – with an average of 3.8 percent of the women enrolled becoming infected each year – despite the gold standard in HIV prevention counseling that was offered as part of the trial, including access to condoms and PrEP, when it became available in the final months of the study.
Along with the need for broader community and social interventions, the study results also highlight the need to refocus efforts to integrate HIV prevention and treatment and family planning programs. Working in concert, both the HIV and family planning communities must do a better job helping women understand their risk of acquiring HIV and how they can protect themselves.
The study also highlights the need for all women, regardless of their risk for HIV, to have access to a range of modern contraceptive methods.
“Although ECHO results are largely reassuring for contraceptive methods included in the trial, a substantial unfinished agenda remains to meet the range of needs of those at risk for unplanned pregnancy and HIV infection, including stronger global and national commitments and accountability for informed choice for family planning and HIV prevention and treatment,” wrote Johns Hopkins University’s Lisa Miyako Noguchi, PhD, in an editorial accompanying the study in the Lancet.
“Many factors are driving unacceptably high rates of HIV acquisition in young women, but we have good reasons to believe that contraception is not one of them.”
CCP has developed a website, Results for Informed Choice, where stakeholders can find tools and resources to help them communicate the ECHO results in a clear and concise way. The website includes a web-based collection of resources and abstracts of relevant peer-reviewed journal articles around the issue to assist country-level decision makers. Additionally, there are statistics on HIV prevalence, HIV incidence and rates of modern family planning method use as well as a timeline of key events, a news feed and a dedicated section for journalists.
James Kiarie, MD, of the World Health Organization, appearing today at the South African AIDS Conference in Durban where the ECHO findings were announced, called the results “reassuring” with regards to contraception, but said it is imperative that HIV prevention efforts be stepped up, especially for young women.
Based on the results of ECHO, and other newly available research, WHO is expected in August to issue updated recommendations through newly issued guidance on contraceptive use for women at high risk of HIV.