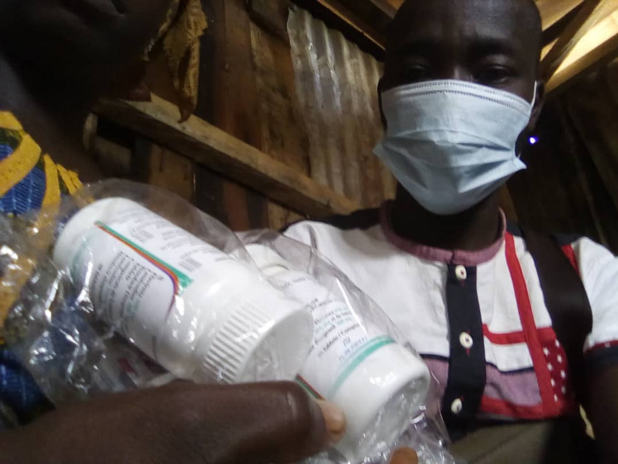
Before the COVID-19 pandemic, the most common way to get antiretroviral therapy (ART) in Côte d’Ivoire was to go to the health center every month. Now, the Johns Hopkins Center for Communication Programs is bringing it directly to the homes of people living with HIV.
As in many places around the world, the pandemic has meant dramatic changes to life in Côte d’Ivoire, changing the way people gather and interact. The spread of rumors and COVID in communities has created fear, keeping people from visiting health facilities for HIV treatment.
“While COVID-19 has hit many communities hard, we have been flexible and found new ways to support those in need with life-saving drugs and adherence support in spite of new restrictions in Côte d’Ivoire,” says Lynn Van Lith, who supports HIV work for CCP.
In Côte d’Ivoire, CCP’s Breakthrough ACTION project supports the national AIDS program by promoting social and behavior change to prevent HIV transmission, encouraging HIV testing and supporting 1,310 people living with HIV. Much of the work has involved peer navigators who are trained to provide in-person services and help people living with HIV to interact with the health care system.
One goal is to make sure that people living with HIV access and stay on their antiretroviral therapy, which is more important than ever during the pandemic. While there is no cure for HIV, antiretroviral therapy can control the virus and prevent sexual transmission to other people.
To make this happen, peer navigators have taken their activities virtual and are now communicating via mobile phone or over WhatsApp to continue addressing concerns about everything from how to prevent COVID-19 to refilling prescription for antiretroviral therapy. Previously, people living with HIV might travel to a faraway health center. Now, peer navigators are arranging community pickup spots and at-home delivery of three months’ supply of medication.
“COVID-19 has inadvertently created an environment that has allowed our peer navigators to build even greater trust with the people they support,” Van Lith says. “Their regular phone calls are a reminder that somebody cares about their well-being and wants them to stay healthy.”
A 30-year-old client says the delivery option for medication has been a blessing. “If you hadn’t come to give me my medicines, I would have taken several more days to get it, even though it’s already been days since I’ve been called to pick it up,” he says. “And then it costs me a lot because I take a taxi to get there and come back.”
The World Health Organization recently developed guidance for countries on how to safely maintain access to essential health services during the pandemic, including for all people living with or affected by HIV. The guidance encourages countries to limit disruptions in access to HIV treatment through “multi-month dispensing,” a policy whereby medicines are prescribed for longer periods of time – up to six months. Côte d’Ivoire is one of the countries now implementing this approach nationally through community-based health workers, such as peer navigators.
Since January, the novel coronavirus has sickened nearly 20 million people across the globe and has killed more than 715,000 people. Pandemic-related lockdowns and other preventive measures have limited the ability of many programs in family planning, malaria, HIV and more to conduct business as usual.
In Côte d’Ivoire, people taking antiretroviral therapy are being asked how they would like to receive their medication. More than 530 of the 1,310 people living with HIV who are served by CCP have opted to get them at home, while the remainder have received them at central locations in their communities.
While the pandemic accelerated plans for community-based distribution, the latest guidance from the President’s Emergency Plan for AIDS Relief (PEPFAR) and the national AIDS program indicate that community-based distribution of antiretroviral therapy is the wave of the future in the fight to eliminate HIV in Côte d’Ivoire.