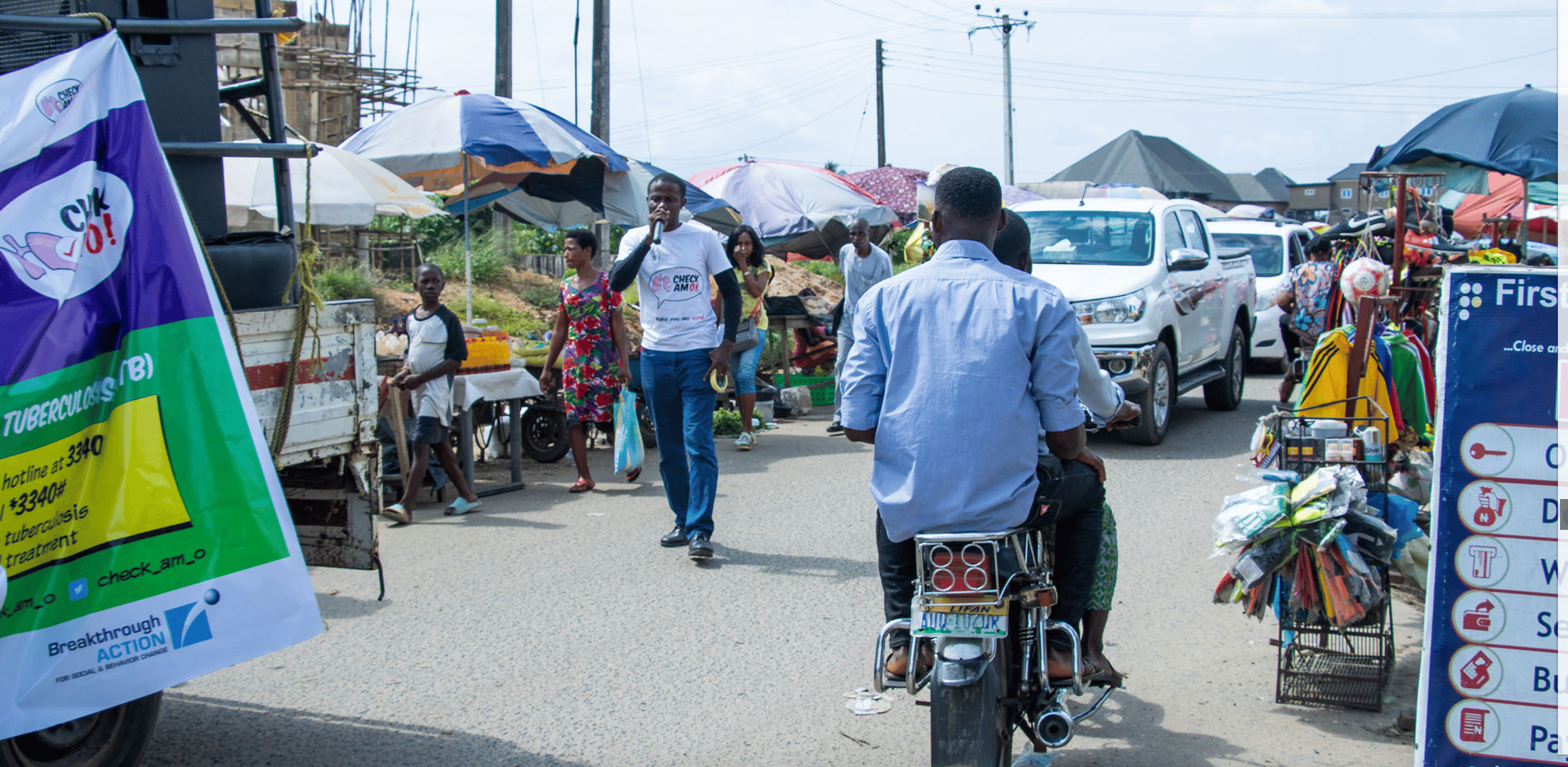For a decade – from 2008 to 2018 – the number of Nigerians diagnosed with tuberculosis and receiving treatment hovered around 100,000 a year. With more than 200 million people, Nigeria has the highest TB burden in Africa, but not enough people with TB know they are sick and therefore unwittingly continue to spread the respiratory disease.
Enter the Johns Hopkins Center for Communication Programs-led Breakthrough ACTION project and its work with Nigeria’s National Tuberculosis and Leprosy Control Programme. The USAID-funded project was awarded $4 million over four years to design and implement social and behavior change interventions to increase the demand for free TB services.
“The question has been, where are the missing TB cases?” says CCP’s Bolatito Aiyenigba, deputy project director for tuberculosis for Breakthrough ACTION-Nigeria. “We know the cases are out there and as long as we are not finding them, TB can be transmitted to other people.”
TB testing and treatment has long been available, but few people accessed the services. The system can only work if people understand how and why they should get themselves evaluated, she says.
“We’re doing so much in terms of providing the diagnostics, the medication … but if people don’t appreciate that they need to take up these services, the numbers of cases identified will remain low,” she says.
Following the introduction of Breakthrough ACTION’s Check Am O! campaign in late 2020, which aims to turn everyday Nigerians into cough monitors and increase the awareness that coughs could be a sign of TB, nearly 208,000 Nigerians were identified in 2021 as having the disease and started on treatment – 66 percent more than the year before. In fact, Nigeria was one of the few countries in the world to achieve an increase in cases identified in 2020, during the height of the COVID-19 lockdown and mitigation measures, making this achievement even more impressive.
A lot of the success came from generating demand for TB testing – helping people understand that a cough lasting longer than two weeks can be a sign of TB – and by dispatching vans with attention-grabbing music and a carnival-like atmosphere manned by health workers and volunteers who can do on-the-spot screening and testing while also dispelling myths about TB.
Once detected, TB can be treated with a long course of anti-tubercular medications.
“It’s a game changer,” Aiyenigba says. “We are creating safe spaces where we are attracting large numbers of people to be tested – and ultimately treated – for TB. The group screening and testing gives the impression of social acceptability. I am encouraged and motivated to do more.”
Just this month, Breakthrough ACTION-Nigeria helped the National Tuberculosis Control program hold a national TB testing week and collected countless more sputum samples while collaborating partners conducted mobile chest X-rays where the equipment was available. The efforts are heavily promoted across social media in Nigeria.
Aiyenigba says that in the coming year, Breakthrough ACTION-Nigeria will focus on health care providers, increasing their interpersonal communication skills to improve patient adherence to treatment and involvement in contact tracing.
With COVID a concern since 2020, Aiyenigba says COVID vaccines have been tacked onto many outreach activities as well as HIV testing.
As part of its work with Nigeria’s National Tuberculosis and Leprosy Control Programme, Breakthrough ACTION also helped increase the capacity of the National TB Call Center, including expanding the number of trained operators and obtaining a short code (3340), instead of the 11-digit phone number, to ease recall and enable more effective cross-promotion on the mass media. Also, the locations of the testing and treatment centers in each local government area were made available on social media and also provided via the National TB Call Center.
As a result, the average number of calls per month to the call center increased from 288 between December 2019 and November 2020 to 11,697 from December 2020 to November 2021. The average number of referrals for testing and treatment increased from 54 in a month to 354 a month over the same time periods.
Nasiru Idris is one of the people impacted by the TB campaigns. “I heard adverts on radio about [free] TB treatment for anyone coughing for over two weeks, so I ran to the hospital and was tested positive for TB,” Idris says. “They gave me medications and told me when to take them. Now, my medications are [finished], and I am back to my normal activities.”